Insights leading to new multiple sclerosis drugs from the rat model
The good news was summed up in just one word: “Eureka!” – “I found it,” wrote Irun Cohen in a telegram to his fellow researcher and colleague Hartmut Wekerle at the Max Planck Institute of Immunobiology in Freiburg in 1981. He was referring to his success in an experiment triggering an inflammatory immune disease in the rat brain. Given that the cost of telegrams was based on length, the Israeli scientist refrained from providing any further explanation.

Together with Avi Ben-Nun, Cohen and Wekerle had been researching an immune disease affecting laboratory animals called autoimmune encephalomyelitis and were trying to transmit it from a sick rat to a healthy one. The scientists thought that if they had enough animals with the disease available to them, it would be easier to study its causes and gain insights that could lead to the development of drugs for the treatment of multiple sclerosis in humans.
And that is exactly what happened: Ben-Nun, Cohen and Wekerle’s transmission technique made such a difference to the study of autoimmune diseases of the central nervous system that it led to the development of several new therapeutic approaches. Many of the drugs available to treat the disease today would not exist but for the three scientists’ “Eureka!” moment.
The German-Israeli research team succeeded for the first time in extracting immune cells from the lymph nodes of rats and deliberately reproducing these cells, which are activated by the basic myelin protein (MPB). These misdirected immune cells, which are described as “autoagressive” recognise the protein and then destroy the myelin which envelops the neuron extensions in the brain and spinal cord like a layer of insulation.
When the researchers transmitted the immune cells that target the myelin protein to healthy rats, the rats contracted this so-called experimental autoimmune encephalomyelitis. The scientists initially needed around one million immune cells that recognized the myelin protein to transmit autoimmune encephalomyelitis from one animal to another. Wekerle later succeeded in “breeding” a cell line that was so specific to the myelin protein, that he was able to transmit the disease with only 10,000 cells.
Experimental autoimmune encephalomyelitis: a model system

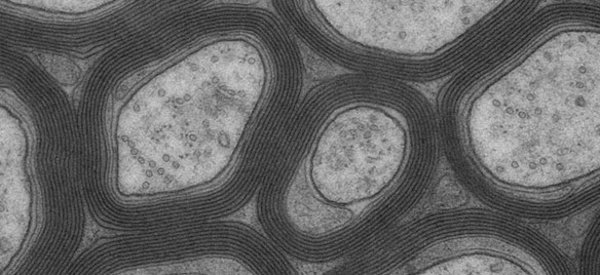
The illustration shows a section of mouse spinal cord under a fluorescence microscope. DMF works on the immune cells (red), which are responsible for damaging the nerve fibres. Cell nuclei appear as blue.
Scientists still trigger experimental autoimmune encephalomyelitis (EAE) in various laboratory animals today, particularly in rats and mice. The main symptoms of the disease are mobility disorders that can extend to paralysis and they are largely the same as the symptoms of multiple sclerosis. For this reason, the disease continues to serve today as a model for the study of multiple sclerosis in humans.
Because the disease places a considerable strain on the affected animals, the scientist, vets and animal carers look after them intensively. If the impacts on the animals are particularly severe, the experiments are abandoned before completion, and the animals are anaesthetized and then destroyed.
Although experimental encephalomyelitis is not entirely comparable with multiple sclerosis and not all treatment approaches derived from it can be applied to humans, the study of this disease has made an important contribution to the development of new treatments for multiple sclerosis. For example, the effect of glatiramer acetate (trade name Copaxone) and natalizumab (Tysabri) were initially tested on animals with experimental autoimmune encephalomyelitis.
Fundamental insights into the immune system

Through the development of their technique, Cohen, Ben-Nun and Wekerle not only made crucial progress in relation to autoimmune encephalomyelitis in animals as a model for the research on multiple sclerosis, with the help of the very same model Wekerle was also able to prove for the first time that “autoreactive” immune cells are kept in check by various control mechanisms which prevent them from reaching their aggressive potential.
Moreover, autoaggressive immune cells can be observed under the microscope following their transmission to the recipient organism. Using a fluorescent dye, scientists can track the migration of the cells from small peripheral blood vessels to the brain in real time. How the immune cells get through the blood-brain barrier is of particular interest to them. It has emerged here that individual cells can only leave the blood vessels in an activated state. Large-scale migration of immune cells to the neural tissue only arises if they find a matching target molecule there.
Another important insight gained from Cohen, Ben-Nun and Wekerle’s work is that a particular type of immune cell plays a crucial role in multiple sclerosis: the T cell. The scientist used these T cells exclusively to transmit the autoimmune encephalomyelitis. For this reason, several drugs of the drugs used today directly target such autoaggressive T cells.
Natalizumab prevents immune cells from penetrating the brain
One such drug is the antibody natalizumab (trade name Tysabri). Its mode of action was initially researched on animals with experimental autoimmune encephalomyelitis. US scientists availed of the technique developed by Cohen, Ben-Nun and Wekerle and discovered through tests on mice and rats that the T cells dock at blood vessel walls with the help of Alpha4 integrin. If they blocked this adhesion protein on the surface of the cell using a substance that later evolved into natalizumab, they were able to prevent the cells from migrating to the brain and the animals remained healthy.
Once natalizumab had been proved to be effective in this model system in animals, it was tested on humans in several clinical studies in the 1990s. The antibody reduced the frequency of permanent damage to the brain by almost 45 percent, and the frequency of flare-ups declined by almost 70 percent.
Natalizumab came onto the market in the USA in 2004. Following its temporary withdrawal due to a fatal complication, natalizumab was licensed again in the USA in 2006 and, finally also in Germany for the treatment of highly active, relapsing multiple sclerosis.


