Inhalation anaesthetics increase the permeability of the blood-brain barrier
Isoflurane could support drug delivery to the brain
In almost all organs, substances can easily pass from circulation into the tissue. Only the brain strongly controls the import of foreign substances. The blood-brain barrier allows only a few substances to enter uncontrolled. One example of such substances is anaesthetics. It has long been suspected that inhalation anaesthetics such as isoflurane affect the blood-brain barrier. A team of scientists at the Max Planck Institute for Experimental Medicine in Göttingen led by Gesine Saher have found that isoflurane switches on an import pathway across the blood-brain barrier. Isoflurane supports chemotherapy of brain tumours in mice. This drug delivery system could be used to treat many diseases of the nervous system.

Blood vessels form a network of supply routes through the brain tissue. A sophisticated system in the blood-brain barrier allows only desired substances such as nutrients to enter the brain. In blood vessels, endothelial cells form tight junctions with each other to prevent the uncontrolled flux of molecules. In addition to acting as a physical barrier, the blood-brain barrier contains numerous transport systems. These ensure the specific import of required substances and the immediate excretion of foreign substances.
While the blood-brain barrier thus ensures optimal performance of the nerve cells under normal conditions, it poses a problem when it comes to diseases of the nervous system (e.g. brain tumours). The strict control of inputs and outputs prevents the import of medications (e.g. chemotherapeutic agents) to the site of action. Despite great research efforts to identify drug delivery tools, pharmacological therapy of brain tumours is often poorly effective. It has long been known that patients can develop neurological deficits after surgery performed under general anaesthesia. "Certain anaesthetics may interfere with brain function by acting on the blood-brain barrier", explains Gesine Saher.
Isoflurane triggers caveolar transport across the blood-brain barrier
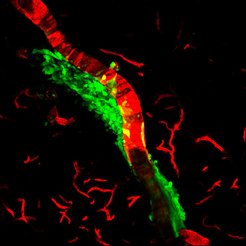
Saher and her working group at the Max Planck Institute for Experimental Medicine in Göttingen investigate the role of cholesterol and other lipids in the nervous system under both physiological and pathological conditions. Together with an international team of researchers from Göttingen, Münster, Oldenburg, and Freiburg, they explored how the inhalation anaesthetic isoflurane affects the membrane lipids of endothelial cells.
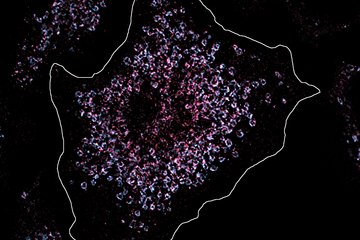
In their study, the researchers used nanoscale microscopy to show that certain membrane areas that are particularly rich in cholesterol were altered by isoflurane. These membrane compartments – also known as "membrane lipid rafts" – can serve as a platform for bulk transport using caveolins. However, this passage is inhibited in the brain. “We wanted to find out whether caveolin-mediated transport is responsible for the increase in blood-brain barrier permeability caused by isoflurane”, explains Lena Spieth, Saher’s colleague and lead author of the study. Indeed, isoflurane exposure failed to increase blood-brain barrier permeability in transgenic mice in which caveolin-1 had been knocked out.
Both the concentration of the anaesthetic and the duration of anaesthesia critically determined the safety of isoflurane application. Prolonged exposure to high dose of isoflurane led to oedema – deposits of fluid around the blood vessels of the brain. When used in moderation, the blood-brain barrier re-established immediately after switching off anaesthesia. “Through the moderate application of isoflurane, we can control the permeability of the blood-brain barrier as if with a switch”, explains Spieth.
Chemotherapy of a brain tumour model was improved by simultaneous isoflurane anaesthesia. “Our results in mice reveal volatile anaesthetics as a new potential factor in the pharmacological therapy of central nervous system diseases”, says Spieth. “Future studies will show whether this treatment can be transferred to humans”, adds Saher, leader of the research team.